Leading killers
“There’s something about chronic illness itself, the illness that doesn’t resolve, that we don’t have adequate cultural narratives for.”
I was taken by this quote from writer and chronic illness advocate Meghan O’Rourke from an interview she did last week. She points out how fragmented healthcare systems and narrative focus on how illness should be ‘overcome’ can leave many patients and conditions without adequate attention.
This discussion has made me think of how we look at excess deaths. Specifically, it has made me think of how mortality may obscure the whole picture of a condition’s impact.
Of course, excess deaths were elevated in the cultural conversation in the earlier days of the COVID-19 pandemic, as we tried to get a grip on the burden of the mass mortality we were experiencing.
However, as anyone familiar with epidemiology knows, excess deaths aren’t just a pandemic issue. They’re a way for us to quantify that mortality burden for a wide variety of conditions or risk factors, including the leading underlying causes of death across a population.
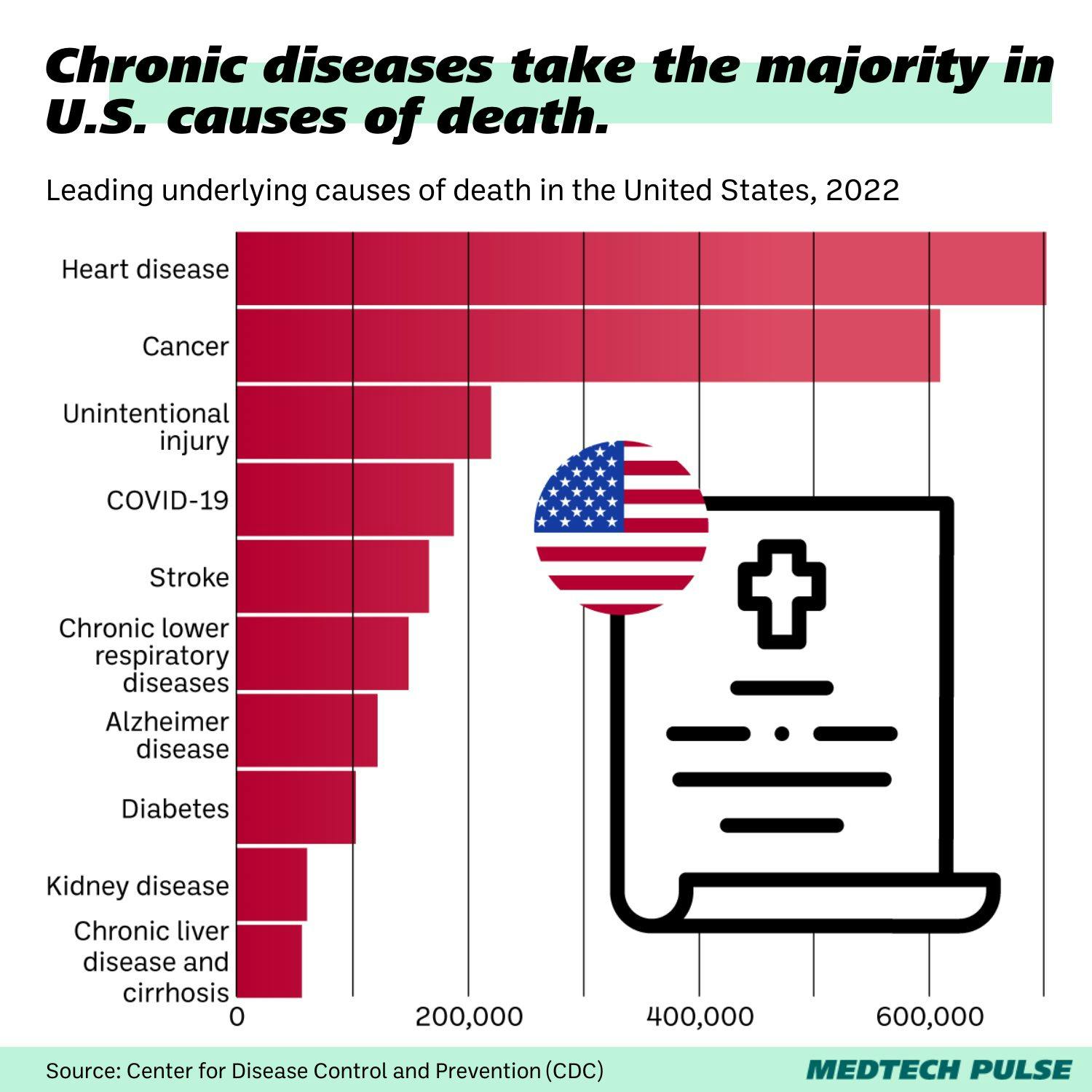
For many examining these numbers, they may seem like an immovable price we must pay. We must resist the temptation to think in this black-and-white way about excess deaths. They are not something we should accept—and they are also not the full picture.
In my view, excess deaths quantify failures of healthcare systems. They point to crises governments and industry must doggedly tackle.
I’m very proud that MedTech Pulse covers innovative solutions that I believe will curb excess mortality across many of these top killers. These include:
- Algorithms targeting underdiagnosed heart disease
- Devices lowering barriers to cancer screening
- Breathtaking advances in precision medicine.
Many of the most exciting advancements aim to find and fight disease at an earlier point in its progression, like the wearable Parkinson’s disease diagnostic sensors covered in the lead article this week.
However, in our drive to prevent excess mortality, we must be careful to not brush another issue under the rug: chronic illness. Just because patients continue living with their disease does not mean that healthcare hasn’t failed them, as O’Rourke commented.
Like we’ve seen with COVID, leading causes of death can also be leading causes of disability and decreases in overall health. If you take a look at the staggering new Long Covid study results set to be published in The Lancet, you’ll see that the impacts of a deadly disease can be long felt across a patient’s world, even when they survive.
I encourage stakeholders and innovators across our industry to invest in the treatment and detection of chronic diseases, preventive care, and long-term health—even for people who may not be able to fully return to their previous level of health.
The goal of medicine is not just to prevent unnecessary death. It’s to give patients the fullest, healthiest lives they can have while they are alive. We must take that responsibility seriously—we cannot lead patients to assume their illnesses are solely their fault or responsibility.
We must be a team.
