Cancer treatment is overdue for an update
It may seem obvious, but cancer care doesn’t end at screening.
However, screening is one of our best tools in the fight against the disease—since the earlier we catch it, the more effective treatments generally are. You may remember from my letter in an edition of MedTech Pulse from last month, cancer screening is one of my personal passions. It’s one of the easiest ways we have to save many lives from this devastating disease. And as you’ll see in our lead article this week, there continue to be innovations making screening options better and better.
Of course, beyond screening, there’s cancer treatment. And my question to you all this week is: Where’s the innovation here?
For the most part, cancer treatment relies on the same three tools it has used forever: chemotherapy, surgery, radiation. And cancer treatment has a formidable reputation. It can be brutal, illness-inducing, and disfiguring in its own right. If a patient’s tumor doesn’t disrupt their life, treatment quite often will. There’s inevitably a balance patients and their doctors need to strike: How much treatment is worth it or even helpful? The answer can vary for each individual. However, as research and innovation continues in the cancer space, medicine has been able to slowly scale back and change its tune on mainstays of cancer treatment.
The history of breast cancer surgery is a great example. The Halsted radical mastectomy used to be the status quo for breast cancer treatment. The surgery involved removing not just the impacted tissue—not even the whole breast—but also parts of the patient’s chest wall and surrounding lymph nodes. The road to the much less dramatic mastectomies and lumpectomies of today took almost a century.
Now, radiotherapy is undergoing its own revolution as researchers and clinicians question whether this cancer care mainstay is still as broadly needed. Like radical mastectomy, this treatment has been around for a long time. Early radiation therapy began shortly after the discovery of X-rays at the end of the 19th century. As it evolved, the focus has continued to be on how to maintain the treatment’s efficacy in destroying the tumor while minimizing damage to the rest of the patient’s body. There’s no denying that radiotherapy carries with it risks of side effects such as intense fatigue or even more severe complications.
Now, some doctors and researchers describe how the growing consensus is in fact: The best way to reduce damage from radiation therapy is to avoid it overall. With advances in precision surgery, better imaging, more advanced chemotherapy, many oncologists are finding radiation often makes little or no difference in outcomes. Of course, these results vary significantly by cancer. In fact, use of radiation is increasing for patients with more advanced cancer, allowing providers to treat patients who previously may have been considered incurable.
Of course, sometimes where we need cancer care innovation isn’t in the treatment in itself, but in reducing friction between diagnosis and treatment. Cancer treatment delays result in many unnecessary deaths.
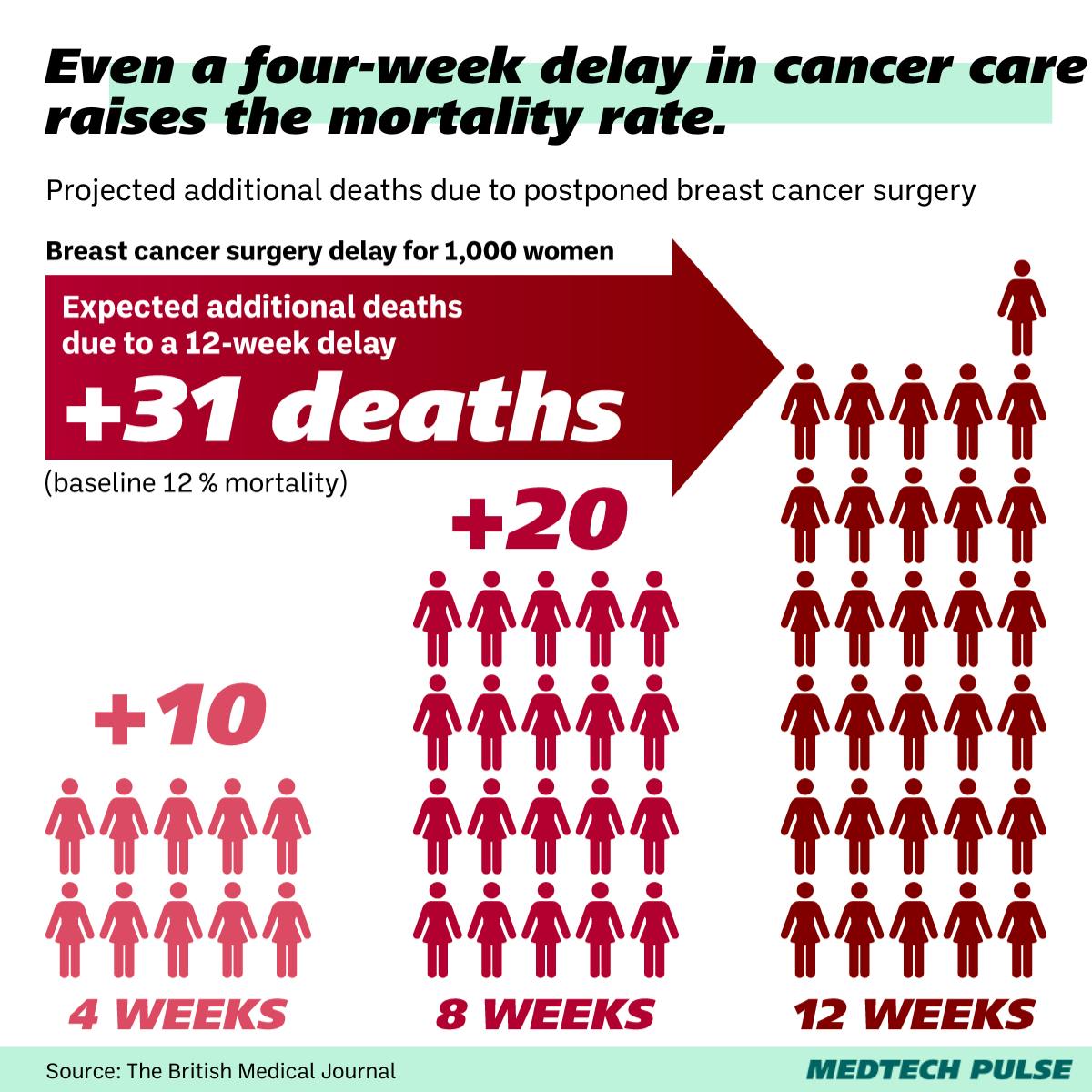
In our modern healthcare system, we must do everything in our power to ensure perfectly curable patients don’t go untreated due to inefficiencies. There’s plenty of room for digital health startup innovation here, especially with AI-enabled automation.
All of this being said, I turn to a broader question: What does it actually take to overcome the status quo in medicine?
It takes drawing inspiration from changes happening in other areas of medicine. You’ll find a great example of this trend in our article this week on using diabetes-inspired precision dosing devices for antibiotic personalization. It also takes dedicating resources to more research on critical conditions. This is how, after many decades, we finally have a blood test for preeclampsia. And in many cases, it’s about battling with cost—once we have an effective new therapy, it’s about making it accessible for the patients who need it.
The work of “disrupting” in medtech goes beyond the work of any individual solution or startup. It’s about moving the needle forward, opening people’s minds to the possibilities. It’s about continuing to dedicate our careers to not accepting a reality where patients can fare better. That’s a mission our whole industry must get behind.
